
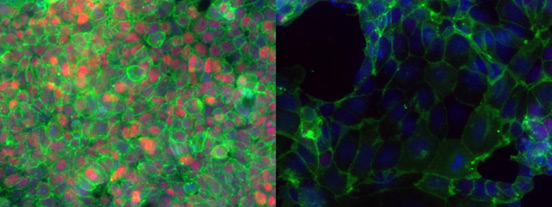
Embryonic stem cells stick together (green, left image) while they express Oct4 protein in their nuclei (magenta, left).
When Oct4 is removed their shape changes and their adhesion to each other is reduced (right panel, nuclei in blue).
(Credit: University of Copenhagen)
Scientists at University of Copenhagen and University of Edinburgh have identified a core set of functionally relevant factors which regulates embryonic stem cells' ability for self-renewal. A key aspect is the protein Oct4 and how it makes stem cells stick together. The identification of these factors will be an important tool in devising better and safer ways of making specialised cells for future regenerative cell therapies for treatment of diseases like diabetes and Parkinson's disease. The results have just been published in the scientific journal Current Biology.
The protein Oct4 plays a key role in maintaining the embryonic stem cells in pure form by turning on stem cell genes, however up until now it has not been know which of the 8,000 or more possible genes that Oct4 can choose from actually support self-renewal.
By comparing the evolution of stem cells in frogs, mice and humans, scientists at the Danish Stem Cell Center (DanStem) and The MRC Centre for Regenerative Medicine in Edinburgh have now been able to link the protein Oct4 with the ability of cells to stick together. They found that for embryonic stem cells to thrive they need to stick together and Oct4's role is to make sure they stay that way.
According to researcher Alessandra Livigni, embryonic stem cells can stay forever young unless they differentiate into grown-up cells. Oct4 can prevent this process by pushing stem cells to stick to each other. The research teams in Edinburgh and Copenhagen successfully identified 53 genes, out of more than 8,000 possible candidates that together with Oct4, functionally regulate cell adhesion. Almost like finding needles in a haystack the scientists have paved the way for a more efficient way of maintaining stem cells as stem cells.
Embryonic stem cell’ pluripotency has great medical potential. However, to be used medically, they need to be maintained as stem cells, until they're needed. When phisicians want to turn a stem cell into a specific cell for example; an insulin producing beta cell, or a nerve cell like those in the brain, they'd like this process to occur accurately and efficiently. They cannot do this if they don't understand how to maintain stem cells as stem cells.
Professor Joshua Brickman has a favourable comment on this new discovery. He said, “This research knowledge has the potential for us to change the way we grow stem cells, enabling us to use them in a less costly and more efficient way. It will help us devise better and safer ways to create specialised cells for future regenerative medicine therapies," concludes Professor Joshua Brickman.”
 H&B
H&B
 Srhealth
Srhealth